- 2487222223
- Mail Us
- Shrigonda, Maharashtra
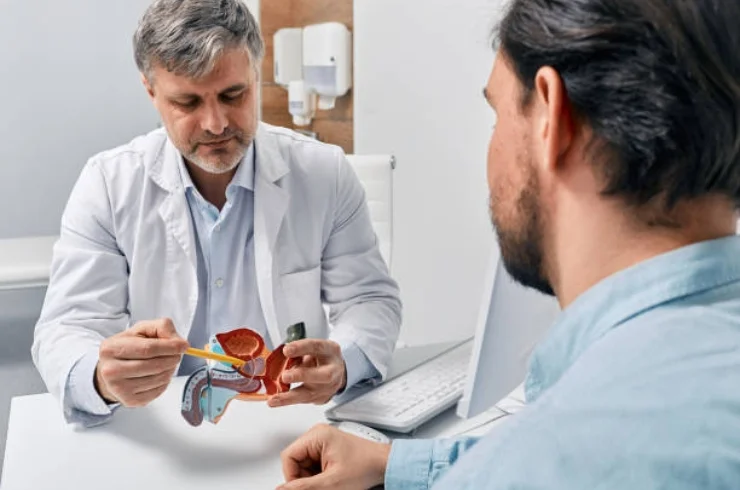
Urology is a medical specialty that focuses on the diagnosis, treatment, and management of disorders related to the urinary tract in both men and women, as well as the male reproductive system. Urologists are trained to deal with a variety of conditions affecting the kidneys, ureters, bladder, urethra, and male reproductive organs.
Urinary Tract Disorders: These include:
Male Reproductive System: Urologists also address issues related to the male reproductive system, including:
Pediatric Urology: Focuses on urinary tract and reproductive system conditions in children, such as congenital abnormalities or urinary incontinence.
Functional Urology: Deals with bladder and urinary function, including issues related to urinary incontinence and pelvic floor disorders.
Urologists utilize various diagnostic methods to evaluate urologic conditions, including:
Urologists often emphasize preventive care through education about risk factors for urinary conditions, the importance of hydration, and regular screenings for prostate health. They also provide guidance on sexual health and reproductive health issues.
Urology is an essential specialty that encompasses a wide range of conditions affecting the urinary tract and male reproductive system. Urologists play a crucial role in diagnosing and treating these disorders, providing both medical and surgical options to help patients improve their quality of life. Advancements in urology continue to enhance treatment options and outcomes for patients with urologic conditions.
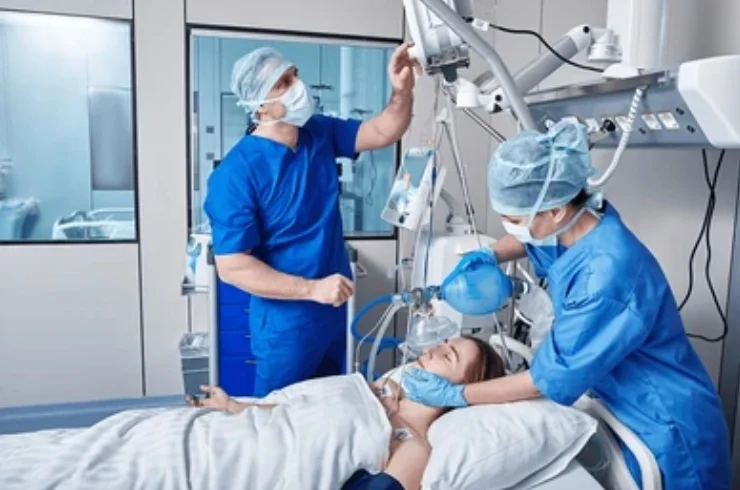
Anaesthesia care is a critical aspect of medical practice, primarily focused on the administration of anaesthesia and the monitoring of patients undergoing surgical and other medical procedures. Anaesthetists, often referred to as anaesthesiologists or nurse anaesthetists, are responsible for ensuring patient safety and comfort during surgery, pain management, and other medical interventions that require sedation.
Preoperative Assessment:
Types of Anaesthesia:
Intraoperative Monitoring:
Postoperative Care:
Pain Management:
Patient safety is the highest priority in anesthesia care. Anaesthetists undergo extensive training to manage potential complications and emergencies. Some risks associated with anaesthesia can include:
Anaesthesia care often involves collaboration with other healthcare professionals, including surgeons, nurses, and anesthesiology assistants. An effective team approach enhances the quality of care and ensures comprehensive management of patients before, during, and after surgical procedures.
The field of anaesthesia is constantly evolving, with advancements in techniques, monitoring technology, and medications that enhance patient safety and comfort. Examples include:
Anaesthesia care is a vital component of modern medicine, encompassing various practices aimed at ensuring patient safety, comfort, and effective pain management during surgical and medical procedures. Anaesthetists play a critical role in the perioperative process, adapting their approach to meet individual patient needs and managing complex situations to minimize risks and enhance recovery. Through continuous advancements in techniques and technology, the field remains committed to improving patient outcomes and ensuring high standards of care.
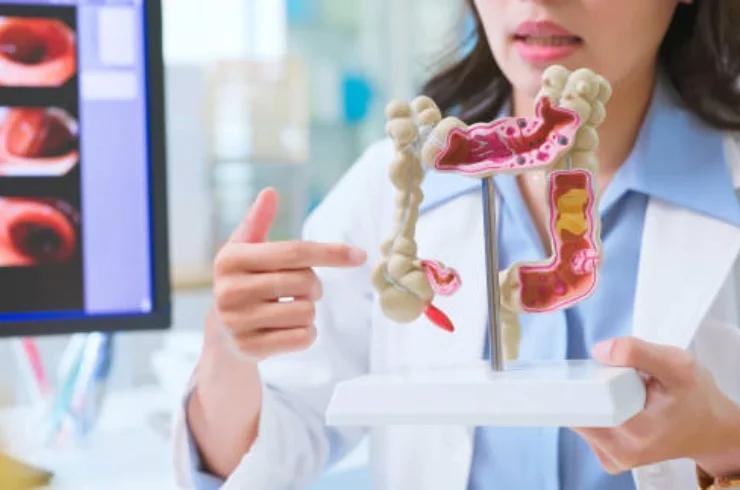
Gastroenterology is a branch of medicine focused on the diagnosis, treatment, and management of disorders of the gastrointestinal (GI) tract, which includes the esophagus, stomach, intestines, liver, gallbladder, pancreas, and bile ducts. Gastroenterologists are specialists trained to deal with a wide range of digestive disorders, with both medical and procedural skills.
Digestive Disorders: Gastroenterologists manage a variety of conditions related to the GI system, including:
Procedures: Gastroenterologists perform several diagnostic and therapeutic procedures, including:
Gastroenterologists use several diagnostic methods to evaluate GI disorders, including:
Gastroenterologists play a critical role in patient education, helping individuals understand their condition, the importance of screening (such as colonoscopy for colorectal cancer), and the management of lifestyle-related factors contributing to GI diseases.
Gastroenterology is a vital specialty that addresses a wide range of digestive diseases and disorders. Through both medical and procedural approaches, gastroenterologists work to improve patients’ digestive health and overall quality of life. Regular screening and early intervention are key components in reducing the morbidity associated with gastrointestinal diseases.
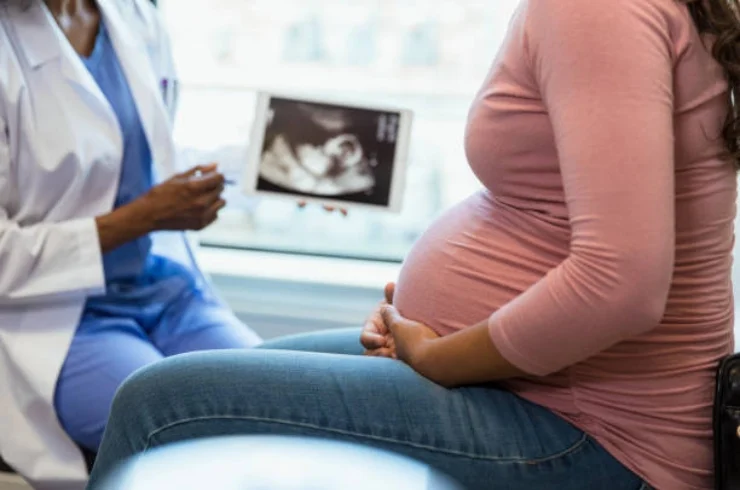
Gynaecology and obstetrics focus on women’s reproductive health, including pregnancy, childbirth, and related conditions. This specialty provides comprehensive care throughout all life stages.
Gynaecology and obstetrics are vital for women’s health, focusing on preventive care and effective treatment to enhance quality of life.
Orthopaedics is a medical specialty dedicated to the diagnosis, treatment, rehabilitation, and prevention of disorders related to the musculoskeletal system. This complex system includes bones, joints, ligaments, tendons, and muscles. Orthopaedic surgeons are trained to treat traumatic injuries, congenital conditions, degenerative diseases, and sports-related injuries, among other issues.
Orthopaedic surgeons perform various surgical procedures, including:
Many orthopaedic conditions can be managed without surgery, including:
Orthopaedics is a vital specialty aimed at maintaining and restoring musculoskeletal health. Orthopaedic surgeons help patients recover from injuries, manage chronic conditions, and improve their quality of life through a combination of surgical and non-surgical treatment options. Their expertise is essential in addressing the wide range of musculoskeletal issues, enabling individuals to regain function and participate in daily activities and sports.
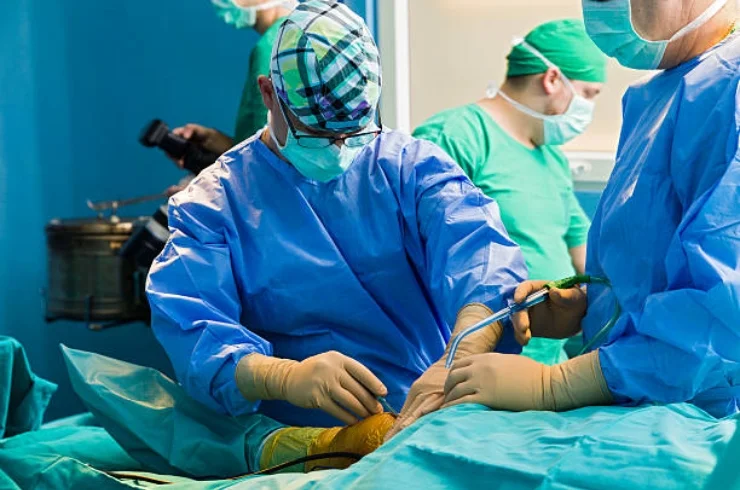
General Surgery is a surgical specialty that focuses on the management of a wide range of surgical conditions, while Laparoscopic Surgery is a minimally invasive surgical technique that allows for procedures to be performed through small incisions using specialized instruments.
General surgeons are trained to perform a variety of surgical procedures and manage surgical patients. Their expertise includes:
Surgical Procedures: General surgeons handle a broad range of operations related to:
Common Conditions Treated:
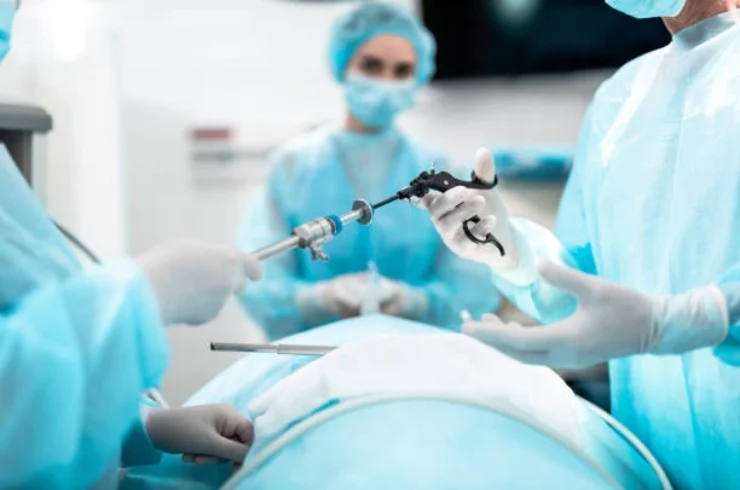
Laparoscopic surgery is characterized by several key features:
Minimally Invasive Technique: It involves using small incisions (usually 0.5 to 1.5 centimeters) instead of large incisions. A laparoscope (a thin tube with a camera) is inserted through one incision to provide visualization of the surgical area, while surgical instruments are inserted through other small incisions.
Benefits of Laparoscopy:
Common Laparoscopic Procedures:
General and laparoscopic surgery represent essential components of the medical field, focusing on the treatment of a wide array of surgical conditions using both traditional and minimally invasive techniques. General surgeons are skilled in managing diverse health issues and play a critical role in surgical care, improving patient outcomes through effective and innovative surgical methods.
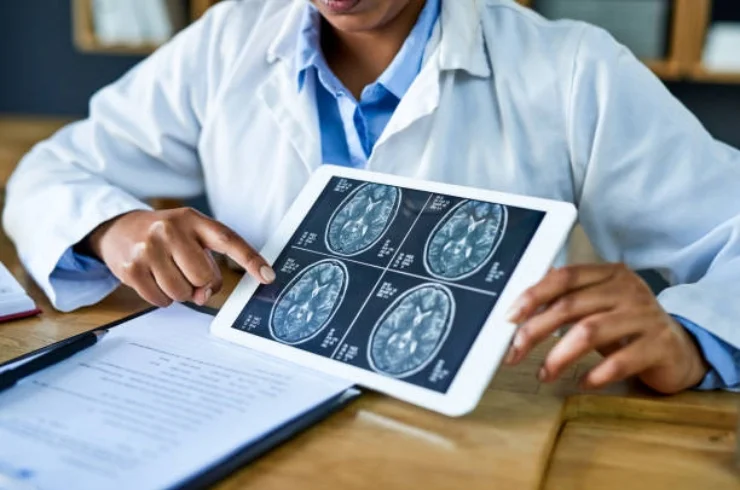
Neurology is a branch of medicine that focuses on the diagnosis, treatment, and management of disorders affecting the nervous system. This includes the brain, spinal cord, nerves, and muscles. Neurologists are specialists who diagnose and treat a wide variety of neurological conditions, employing both medical and therapeutic interventions.
Cerebrovascular Disorders:
Neurodegenerative Diseases:
Seizure Disorders:
Headaches and Migraines:
Multiple Sclerosis (MS): An autoimmune disease affecting the central nervous system, leading to a range of neurological symptoms.
Neuromuscular Disorders:
Neuroinfections:
Neurologists use a range of diagnostic techniques to evaluate neurological conditions, including:
Neurologists often work closely with patients and their families to provide education about neurological conditions, treatment options, and resources for support. They can provide insights into what patients can expect from their conditions and recommendations for managing symptoms.
Neurology is a critical specialty that encompasses a vast range of disorders affecting the nervous system. Neurologists play an essential role in diagnosing, treating, and managing neurological diseases, employing a combination of advanced medical, rehabilitative, and educational strategies to improve patient outcomes and enhance quality of life. As research and technology advance, the field of neurology continues to evolve, bringing new insights and therapies for neurological conditions.
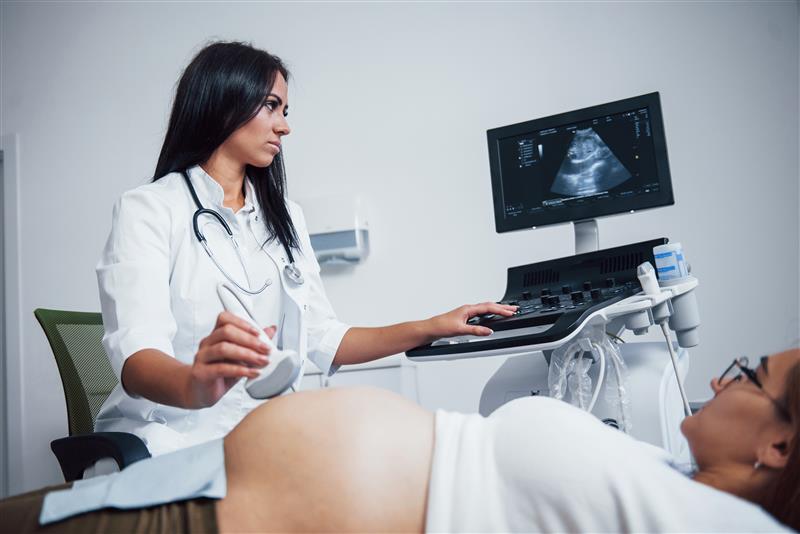
Ultrasound imaging, also known as sonography or ultrasonography, is a medical imaging technique that employs high-frequency sound waves to produce images of organs, tissues, and structures within the body. It is a non-invasive method that is widely used in various medical fields due to its safety, accessibility, and versatility.
Obstetrics and Gynecology:
Abdominal Imaging:
Cardiovascular Ultrasound (Echocardiography):
Musculoskeletal Imaging:
Vascular Imaging:
Pediatric Imaging:
Guided Procedures:
Ultrasound imaging is a versatile and invaluable diagnostic tool in modern medicine, providing critical insights into various conditions across multiple specialties. Its non-invasive nature, absence of ionizing radiation, and ability to provide real-time imaging make it particularly beneficial in obstetrics, cardiology, gastrointestinal medicine, and many other areas. Continued advancements in technology, such as the development of portable ultrasound devices and improved imaging techniques, will likely expand its applications and capabilities in the future.

General Medicine (also known as Internal Medicine) is a medical specialty focused on the prevention, diagnosis, and treatment of a wide range of adult diseases. General internists provide comprehensive care and are often the first point of contact in the healthcare system for adult patients.
General Medicine practitioners utilize various diagnostic methods to evaluate patients, including:
General Medicine serves as a cornerstone of healthcare delivery by:
General Medicine plays a vital role in addressing a broad spectrum of health issues in adults, offering comprehensive and patient-centered care to enhance health outcomes. General internists are pivotal in navigating complex medical conditions, ensuring continuity and coordination of care across the healthcare system.
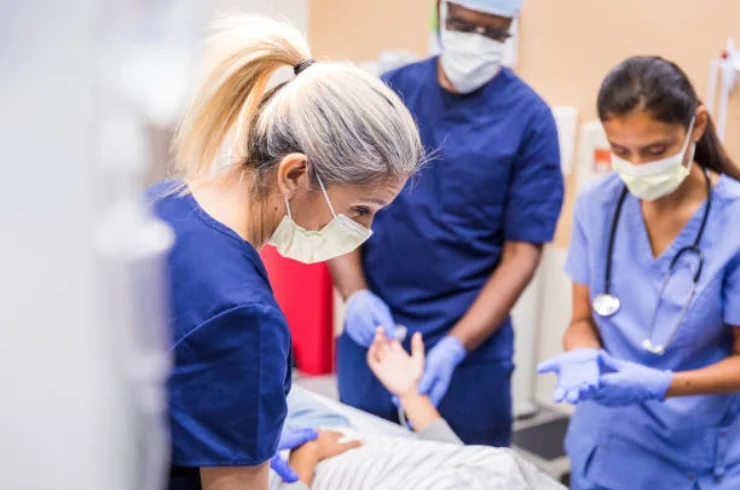
Trauma and critical care medicine focuses on the treatment of severe injuries and critical illnesses, requiring immediate and comprehensive medical attention.
Care in trauma and critical settings often involves collaboration among various specialists, including trauma surgeons, intensivists, nurses, and rehabilitation experts.
Trauma and critical care are essential components of healthcare, providing life-saving interventions and ongoing support to patients with serious injuries and critical conditions. Timely and effective management is crucial for patient recovery and outcomes.
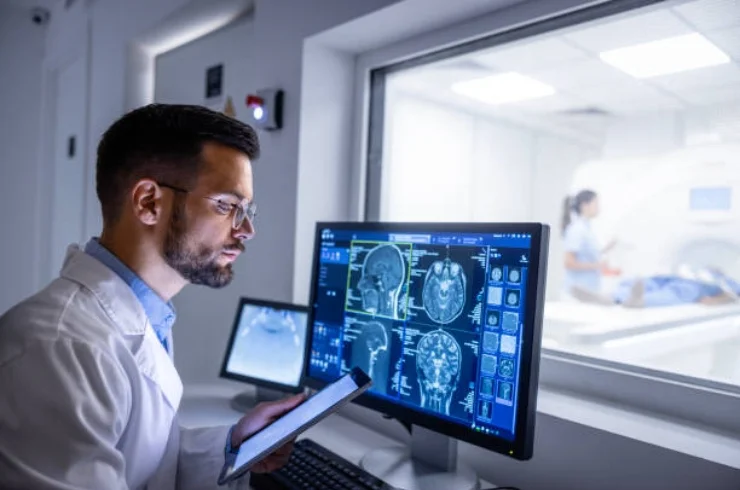
Radiology is a medical specialty that uses imaging techniques to diagnose and treat diseases. Among various modalities, Computed Tomography (CT) scans are a crucial tool for detailed internal imaging.
Radiology, particularly through CT scans, plays a vital role in modern medicine, providing essential insights for diagnosing and treating a wide range of medical conditions. Regular advancements continue to improve imaging accuracy and patient safety.
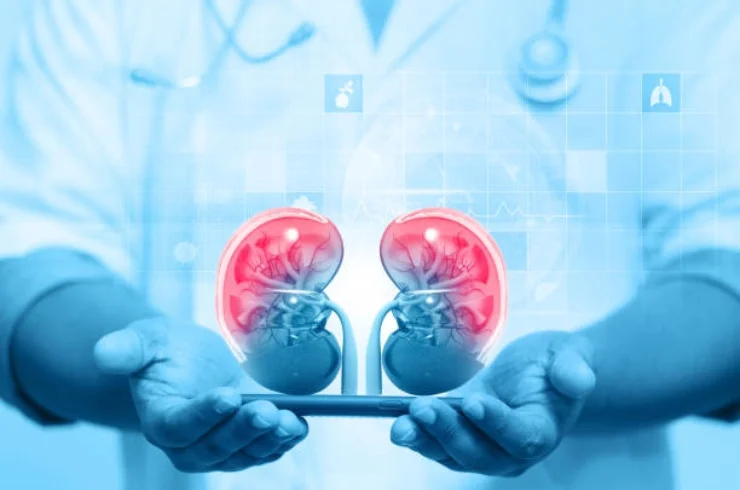
Nephrology is a branch of medicine that deals with the study and treatment of kidney diseases and conditions. Nephrologists specialize in diagnosing, treating, and managing disorders related to kidney function, including urinary system diseases and the broader implications of kidney health on overall well-being.
Diagnosis of Kidney Diseases:
Management of Electrolyte Disorders:
Hypertension Management:
Dialysis and Renal Replacement Therapy:
Patient Education and Lifestyle Modifications:
Preventive strategies in nephrology include:
Nephrology plays a crucial role in managing kidney health and treating associated conditions. Through a combination of early diagnosis, efficient treatment, and patient education, nephrologists work to improve the quality of life for patients with kidney disease and prevent progression to advanced stages requiring dialysis or kidney transplantation. Advances in medical research continue to shape the field, offering new insights and treatment options for patients suffering from kidney-related conditions.
Dedicated to providing comprehensive healthcare services, state-of-the-art facilities, and compassionate support for all patients. Your health and well-being are our top priorities.